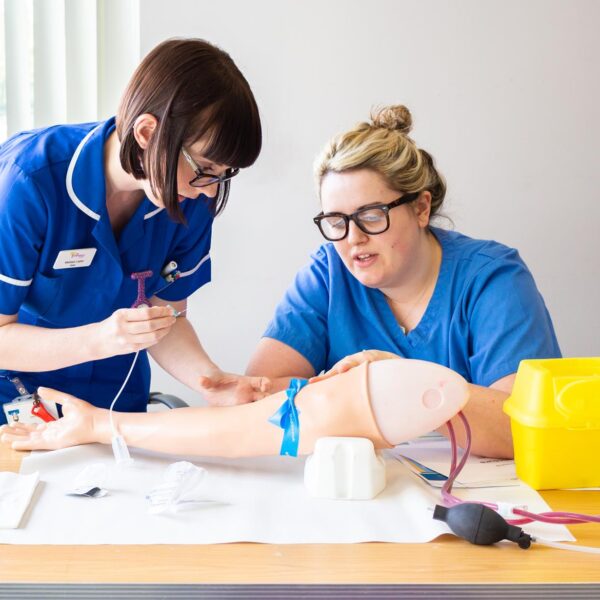
We offer world-class palliative and end of life training and education and carry out research to improve patient care.
The Academic Unit of Palliative Care
The Academic Unit of Palliative Care (AUPC) is a partnership between St Gemma’s Hospice and the University of Leeds.
St Gemma’s is the world’s first University Teaching Hospice. We work to improve care of those approaching the end of life through integrated research, teaching and clinical practice.



Palliative Care Training
We offer a range of a palliative and end of life training and education programmes for healthcare professionals, including free and funded places.

A clear strategic direction
We have ambitious plans for the future. Our AUPC Strategy set out a vision and direction of travel to maintain and grow our centre of excellence.

What we do:
What is a University Teaching Hospice?
St Gemma’s is officially recognised as a University Teaching Hospice – the first hospice to achieve this in the UK and the world.
This prestigious national status reflects our substantial research and teaching activity in collaboration with the University of Leeds, as well as the clinical impact.
We have a long-standing relationship with the University of Leeds and our new status as University Teaching Hospice formally acknowledges the quality of research and teaching our Academic Unit of Palliative Care carries out. It reinforces St Gemma’s position at the forefront of palliative care internationally and will act as the UK benchmark for integrated clinical and academic palliative care.
All of our research, teaching and training is ultimately aimed at improving patient care and means the people we look after will be treated in the best way possible. Whether we are researching pain relief, training students or learning more about palliative care developments across the world, as patients’ needs change over time, we will always be in a position to adapt because of the new research which will be carried out. Our ongoing research ensures St Gemma’s staff and volunteers have the most up-to-date education in standards of care, based on first-hand evidence.
What training do you offer?
We offer a range of a palliative and end of life training and education programmes for all different professionals. Some courses may be in-person at the Academic Unit and others are offered in a virtual or hybrid learning environment. View our current courses .
I am a healthcare professional. How can I study at the Academic Unit of Palliative Care?
We offer a range of palliative and end of life courses for healthcare professionals. You can view and book a course online.
I am an undergraduate/postgraduate student. How can I study at the Academic Unit of Palliative Care?
Please download a clinical placement application form. For more information, please contact training@st-gemma.co.uk.
Can you provide bespoke training for our organisation?
Yes, this is something we may be able to offer. Please contact us on AUPCcourses@st-gemma.co.uk or call us on 0113 218 5500 to discuss your training needs.
Academic Unit of Palliative Care Mission Statement
The AUPC aims to be recognised internationally as a centre of excellence and an outstanding model for improving care of those approaching the end of life through integrated research, teaching and clinical practice.
Our Values
Our work is guided by our values: